The ASAM Criteria, Fourth Edition Adolescents and Transition-Aged Youth Volume
Dedicated treatment standards to improve the health and well-being of youth populations impacted by substance use disorders
Buy Now Read the Announcement
On this Page
Tailored Treatment for Adolescents and Transition-Aged Youth with Substance Use Disorder
The Adolescents and Transition-Aged Youth Volume contains The ASAM Criteria's first dedicated set of treatment standards and program admission criteria for youth populations with a substance use disorder (SUD).
The ASAM Criteria, the most widely used and comprehensive set of standards for addiction treatment programs, promotes individualized and holistic SUD treatment planning. These foundational concepts were combined with the latest research and clinical best practices on adolescent SUD care to create new treatment standards in a dedicated volume that reflect the unique needs of adolescents (youth under 18) and transition-aged youth (ages 16-25) impacted by SUD.
These standards provide a consistent way to:
- Assess a patient's medical, social, and psychological needs to identify an appropriate level of SUD care
- Develop comprehensive, individualized, family-driven and youth-guided treatment plans
- Define the services that should be at each level of care in the continuum of care
The ASAM Criteria, Fourth Edition
Volume 2: Adolescents and Transition-Aged Youth
Digital available March 31, 2026 | Print available June 2026
BUY NOW Read an executive summary
Addiction: A Pediatric-Onset Illness
Severe addiction in adulthood can often be traced back to substance use during childhood. Substance use carries unique risks during adolescence due to the critical brain development that occurs during this stage, making tailored prevention, early intervention, and treatment efforts crucial. The Adolescents and Transition-Aged Youth volume prioritizes these efforts.
Over 80% of adults with SUD initiated substance use before the age of 18.
Those who use substances before age 15 are 6.5x more likely to develop SUD than those who delay use until age 21.
Earlier initiation of substance use is associated with more severe addiction.
Treatment Considerations
Treatment of adolescents and transition-aged youth with SUD have many unique considerations compared with the treatment of adults. These considerations guided the rationale of the volume to support appropriate care for patients.
Developmental Considerations Assessment and treatment services should be adjusted to the adolescent's age and developmental stage. | Co-occurring Conditions Co-occurring mental health conditions are highly prevalent amongst adolescents. These standards expect that all adolescent levels of SUD care provide integrated mental health treatment. |
Family Engagement Children do well when families do well. SUD treatment clinicians should consider a patient's family as part of the unit of care. | Trauma-Sensitive Practices Adverse childhood experiences (ACEs) have profound impacts on the development of SUD. Programs should focus on addressing resulting health consequences from ACEs and build positive childhood experiences that may reduce risk for SUD in adulthood. |
Prevention and Early Intervention The developing adolescent brain is uniquely vulnerable to substance use-related harms. The Adolescent Dimensional Admission Criteria recommends specialty care at Level 1.5Y or 2.1Y for adolescents and transition-aged youth who are using substances and at high risk of SUD but do not currently meet diagnostic criteria. | Transition to Adulthood Substance use can impede development of life skills and attainment of key milestones, like completing education or securing a job. Preparing adolescents for this transition, and the transition to the adult SUD treatment system, is a key theme in this volume. |
Read an executive summary for a comprehensive list of treatment considerations here.
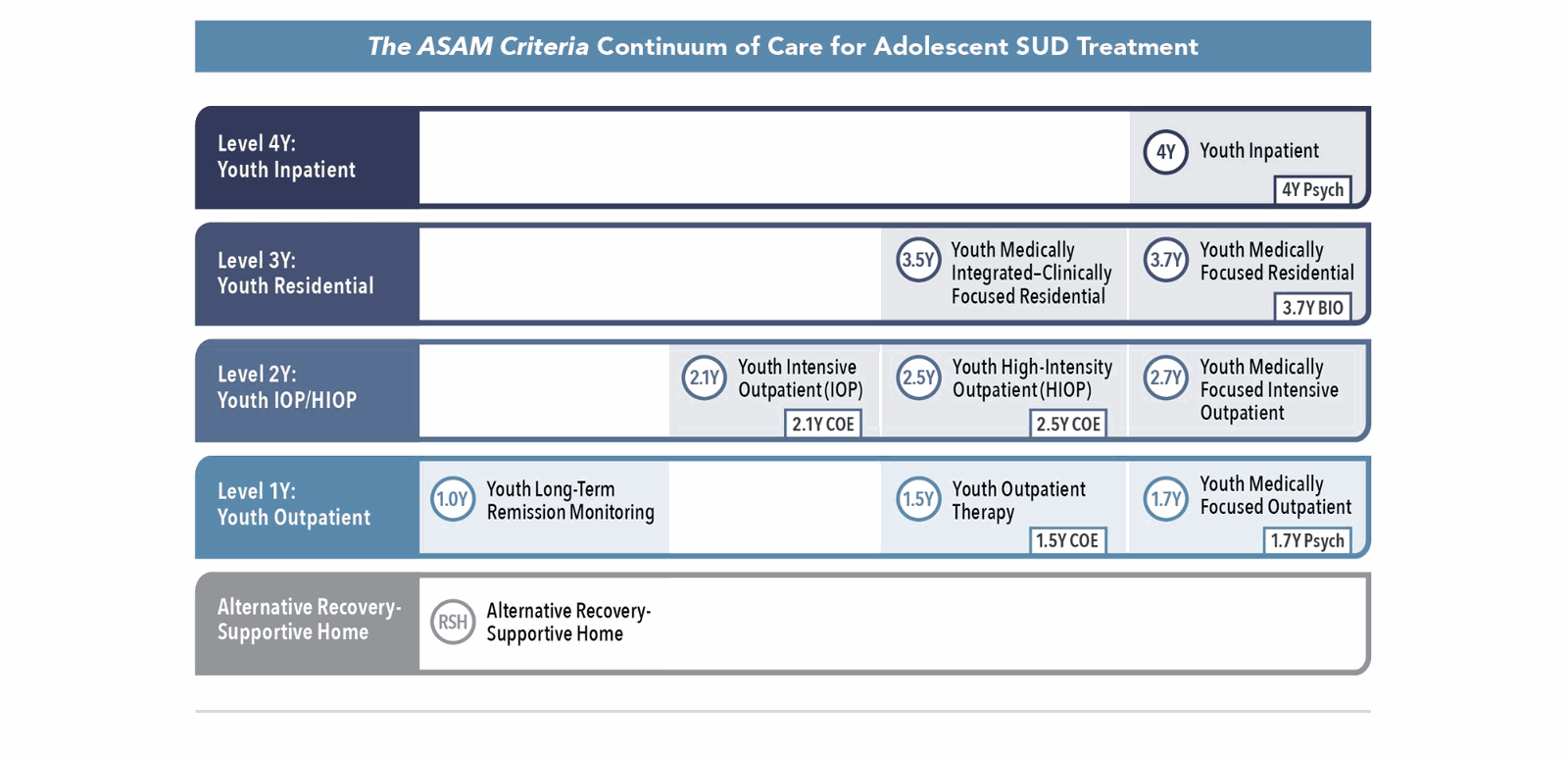
An Adolescent Continuum of Care
The Fourth Edition of The ASAM Criteria describes treatment as a continuum marked by four broad levels of care, with decimal numbers expressing further gradations of treatment intensity.
The updated continuum of care promotes:
- A chronic care model of treatment. The new Level 1.0Y provides ongoing monitoring for adolescents in stable remission, including recovery management checkups and ongoing medication management services for those prescribed addiction medications.
- Co-occurring capable care. In the adolescent continuum of care, co-occurring capability includes providing fully integrated mental health treatment.
- Integration of care. The adolescent continuum of care integrates withdrawal management services in the x.7Y programs with the expectation that these levels also provide integrated biomedical and psychosocial services. It also includes a BIO designation for select Level 3.7Y programs with enhanced biomedical capabilities, including the ability to provide intravenous (IV) fluids and medications, as well as advanced wound care.
- Holistic care. All adolescent SUD treatment programs are expected to provide family services, recovery support services, and risk reduction services. The Fourth Edition of The ASAM Criteria emphasizes the importance of engaging with the patient and family to understand their treatment goals and preferences and being responsive to them.
Dimensions and Subdimensions for Adolescent Assessment
The Fourth Edition describes subdimensions, reflecting core actionable factors, that should be assessed within each dimension. During the Level of Care Assessment, the subdimensions in bold inform level of care recommendations and initial treatment for immediate needs; however, all subdimensions are considered for treatment planning purposes.
Dimension 1: Intoxication, Withdrawal, and Addiction Medications
| Dimension 4: Substance Use-Related Risks
|
Dimension 2: Biomedical Conditions
| Dimension 5: Recovery Environment Interactions
|
Dimension 3: Psychiatric and Cognitive Conditions
| Dimension 6: Person-Centered Considerations
|
Development
These new standards were created using a rigorous methodology for evidence review and consensus development under the guidance of an expert editorial subcommittee.
Editorial Subcommittee
Peter Metz, MD, DLFAACAP, LFAPA (Editorial Advisor)